Why Do My Gums Bleed When I Brush?

Bleeding gums when you brush your teeth are most commonly caused by inflammation of the gums due to plaque buildup (gingivitis). When plaque is not removed properly by brushing and flossing, it irritates the gum tissue, making it swollen, sensitive, and more likely to bleed during brushing or even mild contact. In some cases, bleeding gums can also be a sign of more serious issues such as early gum disease (periodontitis), incorrect brushing technique, vitamin deficiencies, hormonal changes, or certain medical conditions. While occasional mild bleeding can happen, frequent or persistent bleeding should not be ignored, as early treatment can usually reverse the problem and restore healthy gums. Main Causes of Bleeding Gums There is rarely just one reason gums bleed. The causes range from simple mechanical habits to systemic health conditions. Understanding which category applies to you is the first step toward fixing the problem for good. Gingivitis (Early Gum Disease) Gingivitis is the most common cause of bleeding gums. It happens when plaque, a sticky film of bacteria, builds up along the gumline and is not removed properly through brushing and flossing. This leads to gum inflammation, making them red, swollen, and sensitive. In this condition, even gentle brushing can cause bleeding. Since gingivitis is usually painless, many people do not realize they have it until bleeding becomes noticeable. If left untreated, it can progress into a more serious gum condition called periodontitis. Poor Brushing or Flossing Habits Sometimes bleeding gums are caused by the way you clean your teeth. Brushing too hard or using a hard-bristled toothbrush can damage delicate gum tissue and lead to irritation and bleeding. Flossing too aggressively can also cut or injure the gums. On the other hand, not flossing regularly can also cause bleeding when you start again because plaque has already built up between the teeth and caused inflammation. With proper and gentle technique, this usually improves over time. Tartar (Hardened Plaque) Buildup When plaque is not removed in time, it hardens into tartar, which firmly sticks to the teeth and gumline. Unlike plaque, tartar cannot be removed by brushing or flossing at home. It requires professional dental cleaning. Tartar constantly irritates the gums, keeping them inflamed and making them more likely to bleed during brushing or flossing. Vitamin Deficiencies A lack of certain vitamins can also affect gum health. Vitamin C is important for keeping gums strong and helping them heal, and a deficiency can make them weak and more prone to bleeding. Vitamin K is important for blood clotting, so low levels can cause gums to bleed more easily and take longer to stop bleeding even from minor irritation. Hormonal Changes Hormonal changes during pregnancy, puberty, or menopause can make gums more sensitive and reactive. These changes increase blood flow to the gums and affect how the body responds to plaque, making gums more likely to become swollen, inflamed, and prone to bleeding even if oral hygiene habits have not changed. Medical Conditions and Medications Certain medical conditions and medications can also contribute to bleeding gums. Diabetes can weaken the immune system and slow healing, making gum infections more likely. Blood-thinning medications such as aspirin or anticoagulants can also reduce the blood’s ability to clot, which can make gums bleed more easily and for longer periods. Smoking and Tobacco Use Smoking and tobacco use can seriously harm gum health. They reduce blood flow to the gums and weaken the body’s ability to fight infection. Smoking can also hide early signs of gum disease by reducing visible bleeding, which may make the problem seem less serious while it is actually getting worse underneath. Early Warning Signs You Should Not Ignore Bleeding is often the first domino to fall, but it rarely stands alone. Pay close attention to these accompanying signs; they indicate that your gum health needs professional evaluation sooner rather than later. Red, swollen, or tender gums Healthy gums are firm and light pink. If your gums look red, puffy, or feel sore when touched, it usually means there is inflammation caused by plaque buildup along the gumline. This is often one of the earliest signs that gum health is starting to decline. Persistent bad breath Bad breath that does not go away even after brushing or using mouthwash can be caused by bacteria trapped in infected gum areas. This type of odor usually comes from ongoing gum infection. It is a common sign that bacteria are actively growing below the gumline. Gum recession (teeth appear longer) If your gums start pulling away from your teeth, the roots become exposed, making your teeth look longer. This is often a sign of gum disease progressing and weakening gum support. It can increase tooth sensitivity and make teeth more vulnerable to damage. Bleeding that happens daily or worsens Bleeding gums are often the first sign of a problem, but they are usually not the only one. Other symptoms can help you understand when your gums need professional care. These signs often mean that inflammation is already developing and should not be ignored. When Bleeding Gums Become a Serious Problem Bleeding gums may start as a mild issue, but they can become serious if the underlying cause is not treated. Early care is important to prevent long-term damage to your gums and teeth. Progression from gingivitis to periodontitis Gingivitis, while unpleasant, is reversible. But without treatment, it can progress into periodontitis, a more serious form of gum disease. In periodontitis, the infection spreads below the gumline. The body’s immune system, while trying to fight the bacteria, ends up damaging the bone and connective tissue that hold teeth in place. Risk of bone loss and tooth loss Periodontal bone loss is one of the leading causes of tooth loss in adults, not cavities, as many people think. As the bone breaks down, teeth become loose, shift position, and may eventually need to be removed. Infection spreading below the gumline Advanced gum disease creates deep pockets between the teeth and gums where bacteria
Is Gum Disease Hereditary?
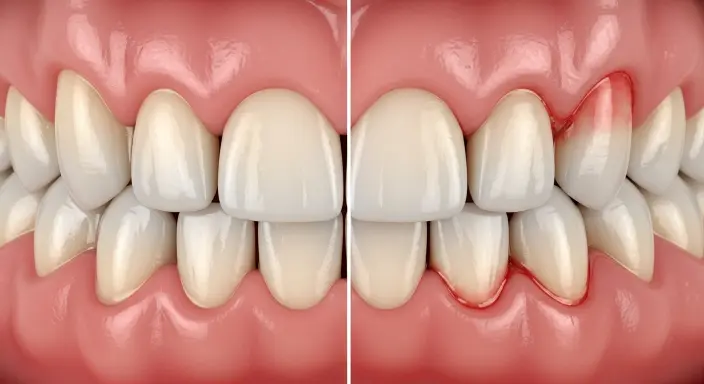
Gum disease can be influenced by genetics, but it is not solely determined by your DNA. While having a family history may increase your susceptibility, lifestyle factors such as oral hygiene, diet, smoking, and overall health play a critical role in whether you develop the condition. If one or both of your parents have experienced gum disease, it’s important to be proactive with regular dental checkups, professional cleanings, and proper at-home oral care. Residents in San Tan Valley, AZ can work with their local dentist to develop a personalized plan for managing hereditary risk. What Is Gum Disease? Gum disease, or periodontal disease, is a bacterial infection affecting the tissues that support your teeth. It begins when plaque, a sticky film of bacteria, is not properly removed through regular brushing and flossing. Over time, this buildup causes inflammation, which can progress from mild, reversible gum irritation to a severe infection that damages the bone and connective tissue holding your teeth. Gingivitis vs. Periodontitis Gum disease exists on a spectrum, from mild gingivitis to advanced periodontitis. Gingivitis: The earliest stage, limited to gum tissue, causes redness, swelling, bleeding, and mild tenderness. It is fully reversible with proper oral hygiene and professional cleaning, with no permanent damage if caught early. Periodontitis: Develops if gingivitis is untreated, spreading below the gum line and damaging bone and connective tissue. Symptoms include gum recession, tooth sensitivity, pockets between teeth and gums, loose teeth, persistent bad breath, and in severe cases, tooth loss. Treatment is more involved, and some damage may be permanent. Common Causes of Gum Disease Poor oral hygiene: Plaque that hardens into tartar provides a breeding ground for bacteria. Lifestyle factors: Smoking, high-sugar or nutrient-poor diets, and chronic stress increase risk by weakening gum health and immune response. Systemic health conditions: Diabetes and other health issues can worsen gum disease, creating a cycle where inflammation and high blood sugar feed each other. How Genetics Play a Role in Gum Disease Gum disease risk is influenced by both genetics and lifestyle, making some individuals more susceptible than others. Understanding your family history can help you take proactive steps to protect your oral health and reduce future problems. Even if gum disease runs in your family, proper care and preventive measures can make a significant difference. Can Gum Disease Be Inherited? Research indicates that genetics can play a role in a person’s susceptibility to gum disease. Studies with twins show that identical twins are more likely to have similar patterns of gum disease compared to fraternal twins, suggesting hereditary factors influence how the body responds to oral bacteria. Genetic variations can affect the immune system, gum tissue strength, and the body’s ability to repair damaged tissue. Family history is one of the strongest indicators of risk if your parents had gum disease or lost teeth due to periodontal problems, your own likelihood of developing the condition is higher. Genetics vs. Lifestyle Having a genetic predisposition to gum disease does not guarantee you will develop it. Daily habits such as brushing, flossing, a balanced diet, and regular dental visits play a major role in determining whether the disease actually occurs. Someone with a strong genetic risk who maintains excellent oral hygiene and avoids smoking may never develop significant gum problems. Conversely, poor oral care or unhealthy habits can lead to gum disease even without hereditary risk. Genetics is just one factor, interacting with lifestyle choices to shape overall oral health. Signs You May Be at Higher Risk Even if you practice good oral hygiene, some people are naturally more susceptible to gum disease due to genetic factors or underlying health conditions. Being aware of your personal risk can help you take proactive steps to protect your gums and prevent serious complications. Early Warning Signs Gum disease often develops gradually and without pain in its early stages, making it easy to overlook. Red, swollen, or tender gums that bleed when brushing or flossing are the most common early indicators. Persistent bad breath that doesn’t improve with brushing and gum recession, where teeth appear longer than usual, can also signal early disease. Increased tooth sensitivity, especially to hot or cold, may indicate that the condition is progressing. Noticing any of these signs should prompt a dental visit rather than waiting for your next routine checkup. Considering Your Family History Understanding your family history is a key step in protecting your gum health. Ask relatives if they have been diagnosed with gum disease, had deep periodontal pockets, or lost teeth due to gum problems. Sharing this information with your dentist allows for closer monitoring, early detection, and a preventive care plan. Early intervention is far more effective and less costly than treating advanced gum disease. Preventing Gum Disease for High-Risk Individuals Even if you are genetically predisposed, proactive steps can significantly reduce your risk of developing gum disease. Understanding your personal risk and adopting consistent preventive habits is key to maintaining healthy gums for life. Oral Hygiene Best Practices For those with a hereditary risk of gum disease, consistent oral hygiene is essential. Brush at least twice daily with fluoride toothpaste, using a soft-bristled or electric toothbrush, and focus on the gum line where plaque accumulates most. Daily flossing removes debris between teeth and just below the gum line areas a toothbrush cannot reach. Consistency matters more than the method; cleaning between teeth every day is the goal. Professional cleanings every six months or more frequently for high-risk patients are crucial. Even the best home care cannot remove tartar once it forms, and only a dental hygienist can eliminate it safely. Lifestyle Adjustments Beyond oral hygiene, lifestyle choices play a major role in reducing gum disease risk. A balanced diet rich in fruits, vegetables, lean proteins, and whole grains supports immune function and reduces inflammation, while limiting sugar and processed foods reduces fuel for harmful oral bacteria. Quitting smoking is one of the most impactful changes a patient can make. Smoking worsens gum disease, masks symptoms, and reduces
Can Braces Fix Uneven Gums?

Yes braces can fix uneven gums in certain cases. When the uneven gum line is caused by tooth position, improper eruption, or crowding, orthodontic treatment can gradually reposition the teeth and create a more balanced gum contour. However, in San Tan Valley, AZ, braces have limitations. If uneven gums are caused by excess gum tissue, advanced gum recession, or differences in underlying bone structure, orthodontic treatment alone will not correct the issue. The key to choosing the right solution at a San Tan Valley, AZ dental clinic is an accurate diagnosis, because what appears to be a simple cosmetic concern can have multiple underlying causes, each requiring a different approach. What Are Uneven Gums? Uneven gums refer to a condition where the gum line does not follow a consistent, symmetrical pattern across your teeth. This imbalance can affect how your smile looks and, in some cases, may point to underlying dental or periodontal concerns. What Does an Uneven Gum Line Look Like? An uneven gum line occurs when the gum tissue sits at different heights across your teeth, making some teeth appear shorter or longer than others. Common signs include noticeable height differences between neighboring teeth, a smile that appears asymmetrical, patches of tooth surface that look unusually long or short, or a wavy rather than smooth gum contour. The severity can range from subtle variations to more pronounced differences, depending on the cause. Is It Just Cosmetic or a Health Concern? While an uneven gum line often affects appearance more than health, certain underlying issues may require attention. Cosmetic concerns, like a gummy smile, are generally harmless, but gum recession, overgrowth, or inflammation can expose sensitive roots, increase the risk of decay, and signal periodontal disease. A professional dental evaluation can determine whether the issue is purely aesthetic or requires treatment to protect oral health. What Causes Uneven Gums? An uneven gum line can result from a variety of factors, and understanding the cause is key to finding the right solution. It’s not always just about appearance; some issues may signal underlying dental health concerns, while others are purely cosmetic. Genetics, oral hygiene habits, and even past dental treatments can all influence how your gum line looks. Tooth Position and Misalignment One of the most common causes of an uneven gum line is the position of your teeth. Teeth that erupt too high or too low compared to their neighbors carry the gum tissue with them, creating noticeable height differences. Crowded, rotated, or overlapping teeth can also push surrounding gum tissue into irregular shapes, preventing a smooth, even arch. Over-Eruption of Certain Teeth Over-eruption occurs when a tooth moves vertically beyond its ideal position, often due to the absence of an opposing tooth. This can pull the surrounding gum and bone tissue downward, causing the tooth to appear longer and disrupting the uniformity of the gum line. Gum Overgrowth (Gingival Enlargement) Gingival enlargement happens when gum tissue grows beyond its normal boundaries, covering more of the tooth surface than intended. It can result from chronic inflammation due to plaque buildup or as a side effect of medications such as blood pressure drugs, anti-seizure medications, and immunosuppressants. In these cases, the excess tissue itself, rather than tooth position, creates the uneven appearance. Gum Recession Recession occurs when gum tissue pulls away from the tooth, exposing more of the root. It is commonly caused by periodontal disease, aggressive brushing, or naturally thin gums. Once gum tissue recedes, it does not naturally grow back, leaving teeth more vulnerable to sensitivity and decay. Bone Structure Differences The underlying bone determines where your gums sit. Uneven bone height from natural variation, past trauma, or bone loss due to periodontal disease can create an uneven gum line. Correcting this type of unevenness may require more advanced dental procedures beyond orthodontics or simple gum reshaping. How Do Braces Affect the Gum Line? Braces work by applying controlled, consistent pressure to gradually move teeth through the surrounding bone. Although braces don’t directly shift gum tissue, the gums and supporting bone respond to these movements, which can subtly alter the appearance of the gum line over time. Specific tooth movements, such as intrusion (pushing a tooth deeper into the jaw) or extrusion (pulling a tooth outward), affect how much gum is visible. Orthodontists carefully control these adjustments to ensure both a functional bite and a more balanced, aesthetically pleasing gum line. When Braces Can Fix Uneven Gums Braces are most effective for uneven gums caused by tooth position. They can level teeth that sit too high or low, reduce excess gum display, and straighten crowded or rotated teeth. As the teeth align, the gum tissue naturally reshapes along a smoother, more balanced line, and correcting bite issues can further improve the gum line. Gum line improvements with braces take time and patience. Changes usually become noticeable several months into treatment as teeth gradually reach their ideal positions. Full results are visible once treatment is complete and the supporting bone has remodeled, which can take additional months after braces are removed. Although gradual, the results can be significant and long-lasting for those whose uneven gums are related to tooth alignment. When Braces Cannot Fix Uneven Gums Braces cannot fix uneven gums caused by excess tissue, such as a gummy smile or gingival enlargement. Moving the teeth does not reduce gum overgrowth, and in some cases, orthodontic movement can make it more noticeable. Similarly, advanced gum recession cannot be corrected with braces, and moving teeth without addressing recession first may worsen tissue loss. Braces are also limited when the issue lies in bone structure or genetics. Significant differences in bone height or naturally asymmetrical gum patterns cannot be corrected with orthodontics alone. While braces can improve many alignment-related issues, they cannot change tissue or bone shape that isn’t linked to tooth position. Do Braces Ever Make Uneven Gums Worse? In some cases, braces can make uneven gums worse, especially if gum recession develops or worsens during treatment. Braces create
Why Do All My Teeth Hurt Suddenly?
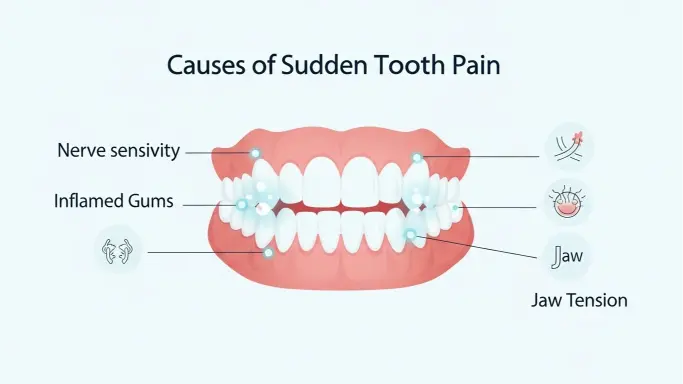
If all your teeth hurt suddenly, the most common causes include tooth sensitivity from enamel loss, sinus infections, teeth grinding, gum disease, or multiple cavities developing simultaneously. Less obvious triggers can include teeth whitening products, acidic foods, or even respiratory infections that create pressure on your tooth roots issues commonly seen by dentists in San Tan Valley, AZ. While some causes of sudden tooth pain are temporary and resolve on their own, others require immediate dental attention—especially if accompanied by swelling, fever, or pain lasting more than 48 hours. Understanding what’s behind your discomfort is the first step toward finding relief and knowing when to see a dentist. Understanding the Sudden Onset of Tooth Pain Sudden tooth pain doesn’t always mean something catastrophic has happened. In many cases, teeth pain all at once develops because of changes in your oral environment, inflammatory responses, or pressure on nerve endings serving multiple teeth simultaneously. Unlike gradual dental problems, sudden onset of tooth pain catches you off guard—often appearing overnight or within hours. The human mouth contains complex networks of nerves that can react quickly to various stimuli. When inflammation occurs in the gums, sinuses, or jaw, pain signals spread throughout your dental structures, making it feel like every tooth is affected. This widespread pain pattern alerts you that something affecting your oral health needs attention. Common Reasons Why All Your Teeth Hurt Suddenly Multiple factors can trigger widespread dental pain, ranging from everyday oral health issues to more complex underlying conditions. Understanding these common causes helps you identify what might be affecting your teeth and when professional care is needed. Let’s examine the most frequent culprits behind sudden, generalized tooth discomfort. Tooth Sensitivity and Enamel Loss Sensitive teeth represent one of the most common reasons for sudden, widespread dental pain. When tooth enamel wears away, the underlying dentin becomes exposed. Dentin contains microscopic tubules leading directly to nerve centers, making teeth extremely reactive to stimuli. Temperature sensitivity ranks among the most recognizable symptoms. You might notice sharp pains when consuming hot coffee or ice cream because thermal changes stimulate nerve endings. Many people find that teeth hurt when eating sweets, as sugar and acidic compounds irritate sensitive nerves. Enamel erosion from acidic beverages, aggressive brushing, teeth grinding, and age-related wear gradually thin enamel, leading to seemingly sudden widespread discomfort. Cavities and Tooth Decay While cavities often affect individual teeth, multiple cavities can develop simultaneously, especially with inconsistent oral hygiene or decay-promoting dietary habits. Tooth decay occurs when bacterial acids eat away at enamel, creating holes that expose sensitive inner layers. Having untreated dental decay across several teeth can cause all your teeth to hurt suddenly. When bacteria penetrate deeper in multiple locations simultaneously, the resulting pain feels widespread and overwhelming. Gum Disease and Receding Gums Gum disease represents a significant cause of generalized tooth pain. When bacteria accumulate along the gum line, they trigger inflammation called gingivitis. If untreated, this advances to periodontitis—a serious gum infection that damages soft tissue and bone. Receiving gums commonly accompany periodontal disease and expose tooth roots that lack protective enamel. Since gum recession can affect your entire mouth, the resulting discomfort makes all your teeth hurt simultaneously. Exposed tooth roots react intensely to temperature changes and touch. Sinus Infection or Sinus Pressure One surprising cause of sudden tooth pain has nothing to do with teeth at all. Sinus infection and sinus congestion can create significant dental discomfort, particularly in upper teeth. Your maxillary sinuses sit directly above the roots of upper molars and premolars. When sinus pressure builds, it pushes downward on tooth roots, creating a dull, aching sensation affecting multiple teeth. The discomfort typically worsens when bending forward or lying down and often occurs alongside facial tenderness, nasal congestion, and headache. Teeth Grinding and Jaw Clenching (Bruxism) Bruxism—teeth grinding and jaw clenching—places enormous pressure on teeth, jaw joints, and surrounding muscles. Many people grind their teeth unconsciously during sleep or clench during stress without realizing it. Teeth grinding wears down enamel, cracks teeth, and irritates ligaments holding teeth in their sockets. When this happens across your dental arch, jaw pain and dental discomfort affect multiple teeth simultaneously. You might wake up with a sore jaw, aching teeth, or headaches from muscular tension. Cracked, Damaged, or Weakened Teeth A cracked tooth doesn’t always announce itself immediately. Hairline cracks might exist before suddenly causing discomfort when bacteria infiltrate or chewing pressure extends the damage. When you have several weakened or damaged teeth, they might all start hurting around the same time. Tooth injury from trauma can affect multiple teeth even if damage isn’t immediately visible. A cracked crown or filling can trigger sudden pain by exposing vulnerable inner tooth structure. Dental Abscess or Infection A dental abscess forms when bacterial infection creates a pus pocket inside or around a tooth. While typically affecting one tooth, dental infection can spread to surrounding tissues, causing pain throughout the affected area. In severe cases, nerve infection radiates beyond the original site. Infection-related tooth pain tends to be intense and throbbing, often accompanied by swelling, bad taste, and fever. An untreated abscess represents a dental emergency because infection can spread to your jaw, neck, and bloodstream. Lifestyle and External Triggers That Can Cause Sudden Tooth Pain Beyond direct dental problems, various lifestyle factors and external influences can trigger sudden, widespread tooth sensitivity. Your daily habits, dietary choices, and oral care routines significantly impact your dental health. These environmental triggers often cause temporary discomfort that resolves once the irritant is removed. Teeth Whitening and Bleaching Products Tooth whitening treatments and teeth bleaching products can cause significant temporary sensitivity. Peroxide-based chemicals penetrate enamel to remove stains but also temporarily make teeth more reactive. Whitening-related sensitivity typically affects all treated teeth since bleaching agent contacts your entire smile. This pain usually appears during treatment or within hours afterward and generally resolves within days after stopping treatment. Acidic Diet and Erosion An acidic diet represents a major contributor to enamel erosion. Beverages like soda,
Can Gum Disease Be Reversed?
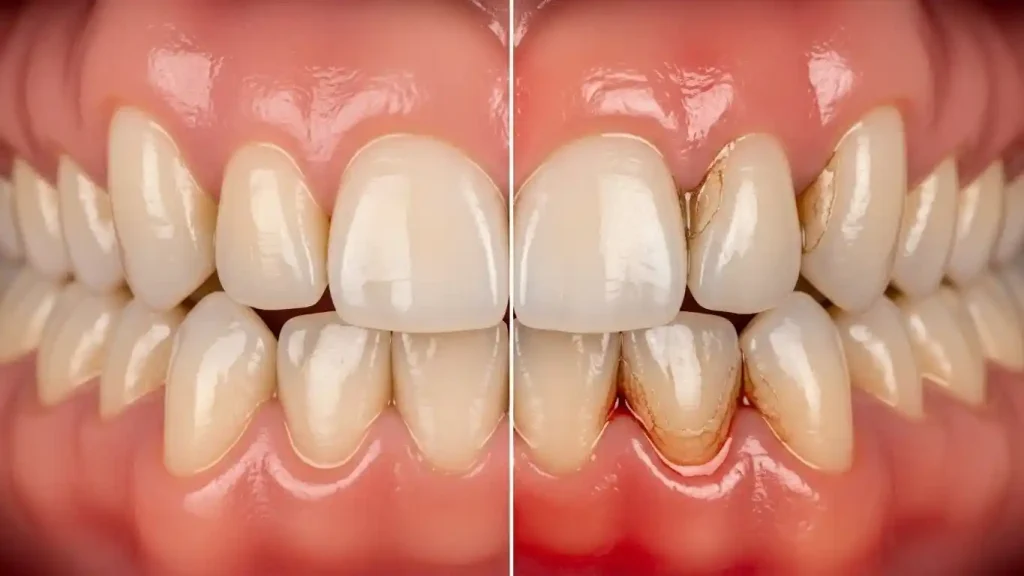
Gum disease is a common problem many people face even when they brush and eat well. The gums around our teeth are more important than many people realize. They help hold our teeth in place, protect the bone underneath, and keep our mouth healthy. When gums become unhealthy, we get gum disease, and this worries a lot of people. The good thing is if gum disease is caught early, it can often be reversed. But if it develops too far, it becomes much harder to fix. In this post, we’ll explain what gum disease is, how it develops, and most importantly when and how it can be reversed. What Is Gum Disease? Gum disease happens when bacteria in your mouth start causing problems for your gums. You know that sticky feeling on your teeth when you wake up in the morning? That’s plaque, and it’s full of tiny bacteria. When you don’t brush and floss well enough, this plaque builds up around your teeth and gums. Think of plaque like a sticky film that sits right where your teeth meet your gums. If you leave it there too long, it turns into something harder called tartar. Your toothbrush can’t remove tartar once it forms. That’s when the real trouble starts because the bacteria in plaque and tartar make your gums angry and swollen. The Two Main Types of Gum Disease Gingivitis: The Early Stage Gingivitis is the first stage of gum disease, and here’s the really important part – it can be reversed! When you have gingivitis, your gums become red and puffy. They might bleed when you brush your teeth or eat something hard like an apple. You might also notice bad breath that doesn’t go away even after brushing. At this stage, the damage is only happening to your gums. The bone that holds your teeth in place is still fine. This is why gingivitis can be turned around if you catch it early and start taking better care of your teeth. Periodontitis: The Advanced Stage If gingivitis doesn’t get treated, it turns into periodontitis. This is much more serious. Now the bacteria have gotten under your gums and started attacking the bone that keeps your teeth in place. This damage is permanent and cannot be completely reversed. When you have periodontitis, your gums start pulling away from your teeth. This creates pockets or spaces between your teeth and gums where more bacteria can hide. These pockets get deeper over time, and regular brushing and flossing can’t reach down there to clean them out. The Four Stages of Gum Disease Understanding the stages helps you know where you stand: Stage 1 – Gingivitis Your gums are red, swollen, and bleed easily. The good news? This stage is completely reversible with proper care. Stage 2 – Early Periodontitis The infection has reached your bone, and you start losing some of it. Your gums might pull away from your teeth by 4-5 millimeters. At this stage, you can stop the disease from getting worse, but you can’t fully reverse the damage. Stage 3 – Moderate Periodontitis More bone is lost, your gums pull away even further (6-7 millimeters), and your teeth might start feeling loose. The pockets around your teeth get deeper and harder to clean. Stage 4 – Advanced Periodontitis This is the most severe stage. A lot of bone is gone, your teeth become very loose, and you might lose teeth. Your gums could have pus, and you’ll probably have constant bad breath. Can Gum Disease Really Be Reversed? Here’s the straight answer: gingivitis can be reversed, but periodontitis cannot be fully reversed. However, even advanced gum disease can be managed and stopped from getting worse. When you have gingivitis, professional cleaning from your dentist plus good brushing and flossing at home can bring your gums back to health. The redness and swelling will go away, the bleeding will stop, and your gums will look pink and healthy again. With periodontitis, you’ve already lost some bone and tissue. That part won’t grow back completely. But you can stop the disease right where it is. Think of it like stopping a leak in your house – you can’t undo the water damage, but you can fix the leak so no more damage happens. Warning Signs to Watch For Pay attention to these signs that might mean you have gum disease: Gums that bleed when you brush or floss Red, swollen, or tender gums Gums that have pulled away from your teeth, making your teeth look longer Bad breath that won’t go away Pus between your teeth and gums Loose teeth or teeth that feel different when you bite Changes in how your teeth fit together when you bite Why Does Gum Disease Happen? The main reason is poor oral hygiene, but other things can make it worse: Poor Brushing and Flossing: When you don’t brush twice a day and floss once a day, plaque builds up fast. After just three days, plaque can harden into tartar. Smoking: This is one of the biggest risk factors. Smoking makes it harder for your gums to heal and weakens your immune system. Diabetes: People with diabetes are more likely to get gum disease. High blood sugar makes it easier for infections to take hold. Genetics: Some people are just more likely to get gum disease because of their genes. If your parents had gum problems, you might too. Stress: When you’re stressed out, your body has a harder time fighting infections, including gum disease. Medications: Some medicines can affect your gums by reducing saliva or making your gums grow bigger. Hormonal Changes: Pregnancy, periods, and menopause can make gums more sensitive and prone to disease. Home Remedies That Can Help If you catch gingivitis early, these home remedies can help alongside good brushing and flossing: Salt Water Rinse: Mix half a teaspoon of salt in warm water and swish it around your mouth for 30 seconds. Do this 2-3 times a
Receding Gums in 20s: Gentle Treatments That Truly Work

You looked in the mirror this morning and noticed your teeth look longer. Your gums have pulled back. You’re only 25 this wasn’t supposed to happen yet. Gum recession felt like something your grandparents dealt with, not you. In this blog post we wil explain why gum recession in 20s happens, what’s causing yours specifically, and what you can actually do to stop it. Is Gum Recession Normal in Your 20s? Short answer: no, it’s not normal. But it’s not rare either.Research shows 10-15% of people in their twenties have visible gum recession. That’s roughly 1 in 7 young adults walking around with this problem right now. You’re not alone. You’re not broken. Something specific is causing it.The difference between recession at 25 versus 65? Older folks accumulate damage over decades. When it hits you young, there’s usually one clear culprit you can identify and eliminate. Your gums aren’t receding because you’re aging. Twenty-five isn’t old. Something else is attacking your gum tissue.Find it. Fix it. Stop the damage. Why Are My Gums Receding in My 20s? Several things trigger early recession. Most people have one or two working against them. Brushing Like You’re Scrubbing a Bathtub This ranks as the top cause in young people. You think harder equals cleaner. It doesn’t.Aggressive brushing strips away gum tissue like sandpaper on wood. The damage accumulates silently for months or years until suddenly you notice teeth looking longer. Check your toothbrush right now. Bristles flattened and bent? You’re pushing way too hard.Get a soft-bristle brush today. Hold it like a pencil, not a weapon. Gentle circles work better than violent back-and-forth scrubbing.Your gums need cleaning, not punishment. Gum Disease Started Years Ago Gum disease in 20s affects 30-40% of young adults. Most don’t know they have it.It begins with gingivitis – puffy, bleeding gums that people ignore. Left alone, it progresses to periodontitis where bacteria eat away at bone supporting your teeth. Plaque forms. Hardens into tartar. Tartar breeds bacteria. Bacteria create infection. Infection destroys tissue.Do your gums bleed when brushing? Warning sign. Even if gums don’t bleed but are receding, chronic infection might’ve been quietly destroying tissue for years. Your DNA Betrayed You Some people inherit thin gum tissue from their parents. Check your family history – if Mom or Dad had gum problems, you’re at higher risk.Thin gums can’t withstand much stress before pulling back. They’re vulnerable by design. You can’t swap your genes. But knowing you’re predisposed helps you take prevention seriously now instead of waiting. Grinding Teeth While You Sleep Wake up with jaw pain? Headaches? Your partner mentions weird grinding noises at night?Bruxism applies enormous pressure to teeth and gums. That constant force pushes teeth out of position and makes gums recede over time. Stress drives grinding. College stress, work stress, relationship drama – your jaw absorbs all that tension while you sleep.A night guard protects everything. Talk to your dentist about getting one fitted properly. Crooked Teeth Create Uneven Pressure Misaligned teeth distribute bite force unevenly. Some teeth take way more pressure than they should handle.That extra force can push teeth slightly out of the bone. Gums follow the teeth and recede as they shift. Orthodontics isn’t just about looking good. Proper alignment protects your gums for decades. Tobacco Is Destroying Everything Smoking or vaping damages gum tissue multiple ways. Reduces blood flow and weakens immune response. Makes infections impossible to fight effectively.Tobacco users face twice the gum disease risk compared to non-users. Smoke chemicals directly kill cells in your gums. Your tissue can’t heal when you’re constantly poisoning it.Quitting is brutal. But gums start healing within weeks of stopping. That Tongue Piercing Isn’t Helping Lip or tongue jewelry rubs against gums constantly. Metal on soft tissue, 24/7, eventually wears everything down.The piercing creates permanent irritation. Friction never stops.If you’ve got piercings and recession in the same spot, there’s your answer. Skipping Dental Cleanings Catches Up Fast Professional cleanings remove tartar you can’t eliminate at home. Tartar sits at your gumline breeding bacteria.Skip appointments and tartar accumulates. Bacteria multiply. Inflammation increases. Gums pull back. Most people need cleanings every six months. Some with gum disease need them every 3-4 months.Those appointments aren’t suggestions if you want healthy gums. How to Tell If You Have Receding Gums Recession happens gradually. You might miss it at first. Watch for these signs:Teeth appear longer than they did last year. Compare current photos to old ones.More tooth surface shows, especially near the gumline. You might see yellow dentin instead of white enamel. A notch forms where gum meets tooth. Run your tongue there – you’ll feel an indent.Temperature sensitivity strikes suddenly. Cold drinks send sharp pain through teeth because roots are exposed. Gums look like they’re pulling away from teeth. The gumline isn’t smooth and even anymore.Food wedges between teeth more easily. Gaps opened up that weren’t there before. What Does Receding Gums Feel Like? Sensations vary wildly between people. Some feel nothing until recession is advanced.Most notice sensitivity first. Cold air on exposed roots creates quick, stabbing pain. Brushing certain teeth becomes uncomfortable. You might feel roughness when running your tongue along the gumline. The smooth transition from tooth to gum gets irregular.Some describe a “tight” sensation, like gums are stretched too thin. Others notice zero feeling but see visual changes. Don’t wait for pain. By the time recession hurts, it’s often progressed significantly. Is Gum Recession Common? The Numbers Gum recession affects roughly 50% of people by age 30. By 50, it hits 88% of people.But most of that happens to older adults who’ve accumulated decades of damage. Specifically among people in their twenties: 10-15% have noticeable recession 30-40% have early gum disease that’ll lead to recession Up to 50% brush too aggressively and face future risk The advantage of catching it at 23 versus 53? You can stop progression before serious damage occurs.Older people often can’t reverse their recession. You still can prevent it from worsening and possibly regrow tissue with treatment. What Age Do
