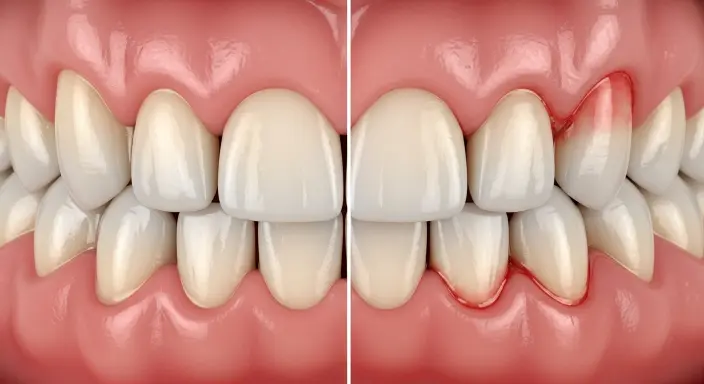
Bleeding gums when you brush your teeth are most commonly caused by inflammation of the gums due to plaque buildup (gingivitis). When plaque is not removed properly by brushing and flossing, it irritates the gum tissue, making it swollen, sensitive, and more likely to bleed during brushing or even mild contact.
In some cases, bleeding gums can also be a sign of more serious issues such as early gum disease (periodontitis), incorrect brushing technique, vitamin deficiencies, hormonal changes, or certain medical conditions. While occasional mild bleeding can happen, frequent or persistent bleeding should not be ignored, as early treatment can usually reverse the problem and restore healthy gums.
Main Causes of Bleeding Gums
There is rarely just one reason gums bleed. The causes range from simple mechanical habits to systemic health conditions. Understanding which category applies to you is the first step toward fixing the problem for good.
Gingivitis (Early Gum Disease)
Gingivitis is the most common cause of bleeding gums. It happens when plaque, a sticky film of bacteria, builds up along the gumline and is not removed properly through brushing and flossing. This leads to gum inflammation, making them red, swollen, and sensitive.
In this condition, even gentle brushing can cause bleeding. Since gingivitis is usually painless, many people do not realize they have it until bleeding becomes noticeable. If left untreated, it can progress into a more serious gum condition called periodontitis.
Poor Brushing or Flossing Habits
Sometimes bleeding gums are caused by the way you clean your teeth. Brushing too hard or using a hard-bristled toothbrush can damage delicate gum tissue and lead to irritation and bleeding. Flossing too aggressively can also cut or injure the gums.
On the other hand, not flossing regularly can also cause bleeding when you start again because plaque has already built up between the teeth and caused inflammation. With proper and gentle technique, this usually improves over time.
Tartar (Hardened Plaque) Buildup
When plaque is not removed in time, it hardens into tartar, which firmly sticks to the teeth and gumline. Unlike plaque, tartar cannot be removed by brushing or flossing at home. It requires professional dental cleaning. Tartar constantly irritates the gums, keeping them inflamed and making them more likely to bleed during brushing or flossing.
Vitamin Deficiencies
A lack of certain vitamins can also affect gum health. Vitamin C is important for keeping gums strong and helping them heal, and a deficiency can make them weak and more prone to bleeding. Vitamin K is important for blood clotting, so low levels can cause gums to bleed more easily and take longer to stop bleeding even from minor irritation.
Hormonal Changes
Hormonal changes during pregnancy, puberty, or menopause can make gums more sensitive and reactive. These changes increase blood flow to the gums and affect how the body responds to plaque, making gums more likely to become swollen, inflamed, and prone to bleeding even if oral hygiene habits have not changed.
Medical Conditions and Medications
Certain medical conditions and medications can also contribute to bleeding gums. Diabetes can weaken the immune system and slow healing, making gum infections more likely. Blood-thinning medications such as aspirin or anticoagulants can also reduce the blood’s ability to clot, which can make gums bleed more easily and for longer periods.
Smoking and Tobacco Use
Smoking and tobacco use can seriously harm gum health. They reduce blood flow to the gums and weaken the body’s ability to fight infection. Smoking can also hide early signs of gum disease by reducing visible bleeding, which may make the problem seem less serious while it is actually getting worse underneath.
Early Warning Signs You Should Not Ignore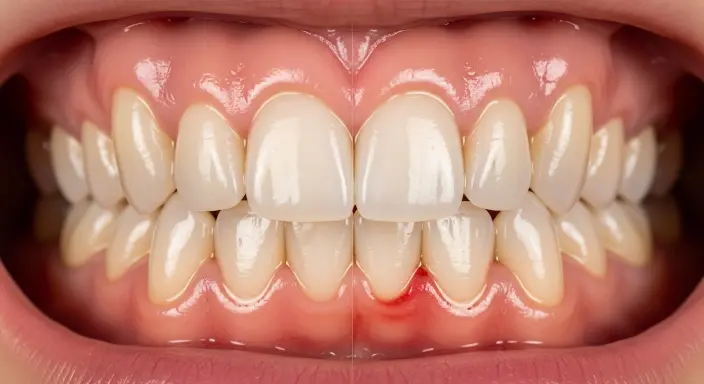
Bleeding is often the first domino to fall, but it rarely stands alone. Pay close attention to these accompanying signs; they indicate that your gum health needs professional evaluation sooner rather than later.
Red, swollen, or tender gums
Healthy gums are firm and light pink. If your gums look red, puffy, or feel sore when touched, it usually means there is inflammation caused by plaque buildup along the gumline. This is often one of the earliest signs that gum health is starting to decline.
Persistent bad breath
Bad breath that does not go away even after brushing or using mouthwash can be caused by bacteria trapped in infected gum areas. This type of odor usually comes from ongoing gum infection. It is a common sign that bacteria are actively growing below the gumline.
Gum recession (teeth appear longer)
If your gums start pulling away from your teeth, the roots become exposed, making your teeth look longer. This is often a sign of gum disease progressing and weakening gum support. It can increase tooth sensitivity and make teeth more vulnerable to damage.
Bleeding that happens daily or worsens
Bleeding gums are often the first sign of a problem, but they are usually not the only one. Other symptoms can help you understand when your gums need professional care. These signs often mean that inflammation is already developing and should not be ignored.
When Bleeding Gums Become a Serious Problem
Bleeding gums may start as a mild issue, but they can become serious if the underlying cause is not treated. Early care is important to prevent long-term damage to your gums and teeth.
Progression from gingivitis to periodontitis
Gingivitis, while unpleasant, is reversible. But without treatment, it can progress into periodontitis, a more serious form of gum disease. In periodontitis, the infection spreads below the gumline. The body’s immune system, while trying to fight the bacteria, ends up damaging the bone and connective tissue that hold teeth in place.
Risk of bone loss and tooth loss
Periodontal bone loss is one of the leading causes of tooth loss in adults, not cavities, as many people think. As the bone breaks down, teeth become loose, shift position, and may eventually need to be removed.
Infection spreading below the gumline
Advanced gum disease creates deep pockets between the teeth and gums where bacteria can grow and cannot be removed by normal brushing. These pockets can hold long-term infections that may spread to nearby tissues and enter the bloodstream in severe cases.
How Dentists Diagnose Bleeding Gums
When you visit a dentist about bleeding gums, they will conduct a thorough assessment rather than making a quick visual judgment. The diagnostic process typically involves several steps.
Gum pocket measurement
Using a small, calibrated instrument called a periodontal probe, your dentist or hygienist will gently measure the depth of the pockets between your gums and teeth at multiple points around each tooth. Healthy pockets measure between 1 and 3 millimeters. Readings of 4 millimeters or more indicate disease, and deeper pockets correlate with more advanced periodontitis.
Checking plaque and tartar levels
The clinician will assess the extent of plaque and tartar accumulation at and below the gumline. This helps them understand how established the infection is and what kind of treatment will be most effective.
Dental X-rays for bone health
X-rays are indispensable for evaluating the bone levels around each tooth. Since bone loss occurs beneath the visible surface of the gums, X-rays give the dentist a clear picture of how much structural support remains and where the disease has progressed most aggressively.
Identifying gum disease stage
Using the data gathered from probing measurements, visual examination, and imaging, the dentist will classify the disease stage. This staging guides the treatment plan everything from a routine professional cleaning to more involved procedures like scaling and root planning.
Professional Treatment Options
Treatment for bleeding gums depends on how severe the condition is. In most cases, early care from a dentist can quickly improve gum health and stop the problem from getting worse.
Routine professional cleaning (removes plaque and tartar)
For mild gingivitis, a professional cleaning (also called prophylaxis) is usually enough. The dentist or hygienist removes plaque and tartar from above and just below the gumline, cleans and polishes the teeth, and checks your brushing and flossing habits. With good home care afterward, gums often return to normal within a few weeks.
Deep cleaning (scaling and root planning)
If gum disease has progressed below the gumline, a deep cleaning is needed. This treatment removes plaque, tartar, and bacteria from deep gum pockets and smooths the tooth roots so bacteria cannot easily return. It is usually done under local anesthesia and may require more than one visit.
Prescription mouth rinses or antibiotics (if needed)
In some cases, a dentist may prescribe a special mouth rinse or antibiotics to help control infection. These are used along with cleaning treatments, not as a replacement for them. They help reduce bacteria and support healing of the gums.
Treating underlying health issues
If bleeding gums are linked to health problems like diabetes, vitamin deficiencies, or medication side effects, those issues also need to be addressed. Dentists often work with your physician because gum health improves best when the overall health condition is also managed.
How to Stop Bleeding Gums at Home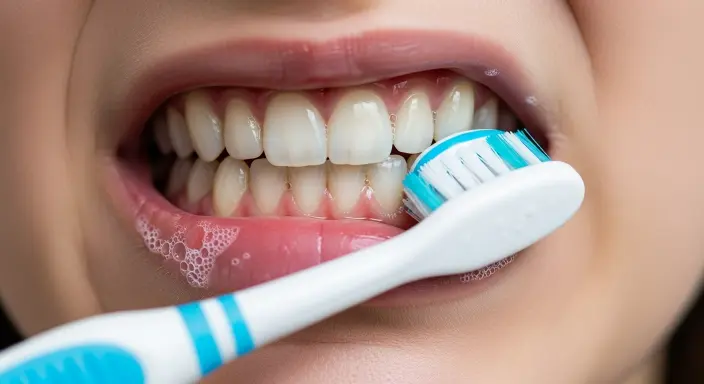
Professional treatment is essential, but the vast majority of gum health maintenance happens at home, every single day. Small, consistent improvements to your routine can make a dramatic difference.
Use a soft-bristled toothbrush correctly
Angle the bristles at 45 degrees toward the gumline, use gentle circular motions, and spend at least two minutes brushing morning and night. Never scrub aggressively. Firm pressure does not equal better cleaning; it just causes damage.
Gentle daily flossing (don’t skip it)
Slide floss between teeth and curve it into a C-shape against the tooth, moving it up and down against the surface so it does not snap or see it into the gums. If your gums bleed initially, keep going. With consistent daily flossing, the bleeding should stop within one to two weeks as the gum tissue becomes healthier.
Anti-gingivitis or fluoride toothpaste
Look for formulas with stannous fluoride specifically targeting gum disease. These provide antibacterial benefits alongside cavity protection and are notably more effective for gum inflammation than standard whitening pastes.
Warm saltwater rinses for inflammation
Dissolve half a teaspoon of salt in a cup of warm water and rinse for 30 seconds after brushing. This simple rinse reduces bacterial load and soothes inflamed tissue without disrupting the oral microbiome the way some antiseptic rinses can with long-term use.
Improve diet (vitamin-rich foods)
Prioritize foods rich in Vitamin C (citrus fruits, bell peppers, leafy greens) and Vitamin K (broccoli, spinach, fermented foods). Reduce sugar and processed carbohydrates, as these feed the bacteria responsible for plaque formation.
Stop smoking and reduce sugar intake
There is no dental intervention that will work optimally as long as tobacco use continues. Quitting smoking is one of the single most impactful steps a person can take for gum health and cutting back on sugar removes the primary fuel source for the bacteria driving the problem.
How to Prevent Bleeding Gums Long-Term
Preventing bleeding gums is mostly about maintaining good daily habits and not allowing plaque to build up in the first place. With consistent care, most gum problems can be avoided completely.
Maintain a consistent oral hygiene routine
Brushing twice a day, flossing daily, and using a gentle mouth rinse helps remove plaque before it can cause irritation. This simple routine keeps bacteria under control and prevents gum inflammation from developing.
Replace your toothbrush every 3 months
Old toothbrushes with frayed bristles clean less effectively and can irritate your gums. Replacing your toothbrush every three months helps maintain proper cleaning and protects gum tissue.
Regular dental checkups every 6 months
Routine dental visits help detect early signs of gum disease before they become serious. Your dentist can monitor your gum health and make sure any issues are treated early.
Professional cleanings to prevent buildup
Even perfect home care cannot remove tartar once it has formed. Regular professional cleanings reset the baseline, removing any deposits that have accumulated and keeping your gum health on track between appointments.
When You Should See a Dentist Immediately
Most bleeding gum situations benefit from improved home care and a scheduled dental visit. But some symptoms warrant urgent attention. Do not wait for your next routine checkup if any of the following apply.
Bleeding lasts more than 7 days
If you have improved your brushing and flossing technique and bleeding continues beyond a week, something beyond poor habits is likely at play. A professional assessment is needed.
Pain, swelling, or pus in gums
These are signs of active infection that require prompt treatment. Pus around the gumline or between teeth is a dental emergency. Do not delay.
Loose teeth or shifting bite
Teeth that feel mobile or a bite that has noticeably changed are signs of significant bone loss. This level of deterioration needs immediate professional evaluation to stop further damage.
Severe bad breath that won’t go away
Persistent, severe halitosis that does not respond to brushing, flossing, or rinsing is often a sign of infection deep within the gum pockets beyond what any home remedy can reach.
Get Expert Gum Care in San Tan Valley, AZ
If your gums bleed when you brush, don’t ignore it. It could be an early sign of gum disease that needs professional care. At San Tan Dentist in San Tan Valley, AZ, our dental team can carefully examine your gums, identify the cause of bleeding, and provide the right treatment to restore your oral health. Book your dental appointment today and get personalized care to stop gum bleeding and protect your smile before the problem gets worse.
Conclusion
Bleeding gums when brushing are usually an early warning sign of gum inflammation caused by plaque buildup. In many cases, it starts as mild gingivitis and can be reversed with proper oral hygiene and timely dental care. However, if ignored, it can progress into more serious gum disease that may lead to bone loss, loose teeth, and long-term oral health problems.
The good news is that bleeding gums are highly preventable and treatable when caught early. With consistent brushing, daily flossing, a healthy lifestyle, and regular dental checkups, most people can restore and maintain healthy gums. If bleeding continues or worsens, it is important to visit a dentist without delay.
Frequently Asked Questions
Why do my gums bleed when I brush my teeth?
Gums usually bleed due to plaque buildup along the gumline, which causes inflammation known as gingivitis. It can also be caused by brushing too hard, flossing incorrectly, or early gum disease.
Is it normal for gums to bleed when brushing?
No, it is not considered normal. Occasional light bleeding may happen if you have not flossed in a while, but frequent or daily bleeding is a sign of gum problems that should be checked.
How can I stop my gums from bleeding?
You can stop bleeding gums by brushing gently twice a day, flossing daily, using an antibacterial toothpaste or mouth rinse, improving your diet, and visiting your dentist for a professional cleaning.
Can bleeding gums be a sign of serious disease?
Yes, in some cases bleeding gums can indicate advanced gum disease (periodontitis), diabetes-related gum issues, or vitamin deficiencies. That is why persistent bleeding should not be ignored.
How long does it take for bleeding gums to heal?
With proper oral care, mild gingivitis-related bleeding can improve within 1 to 2 weeks. If it continues beyond that, professional dental treatment is usually needed.