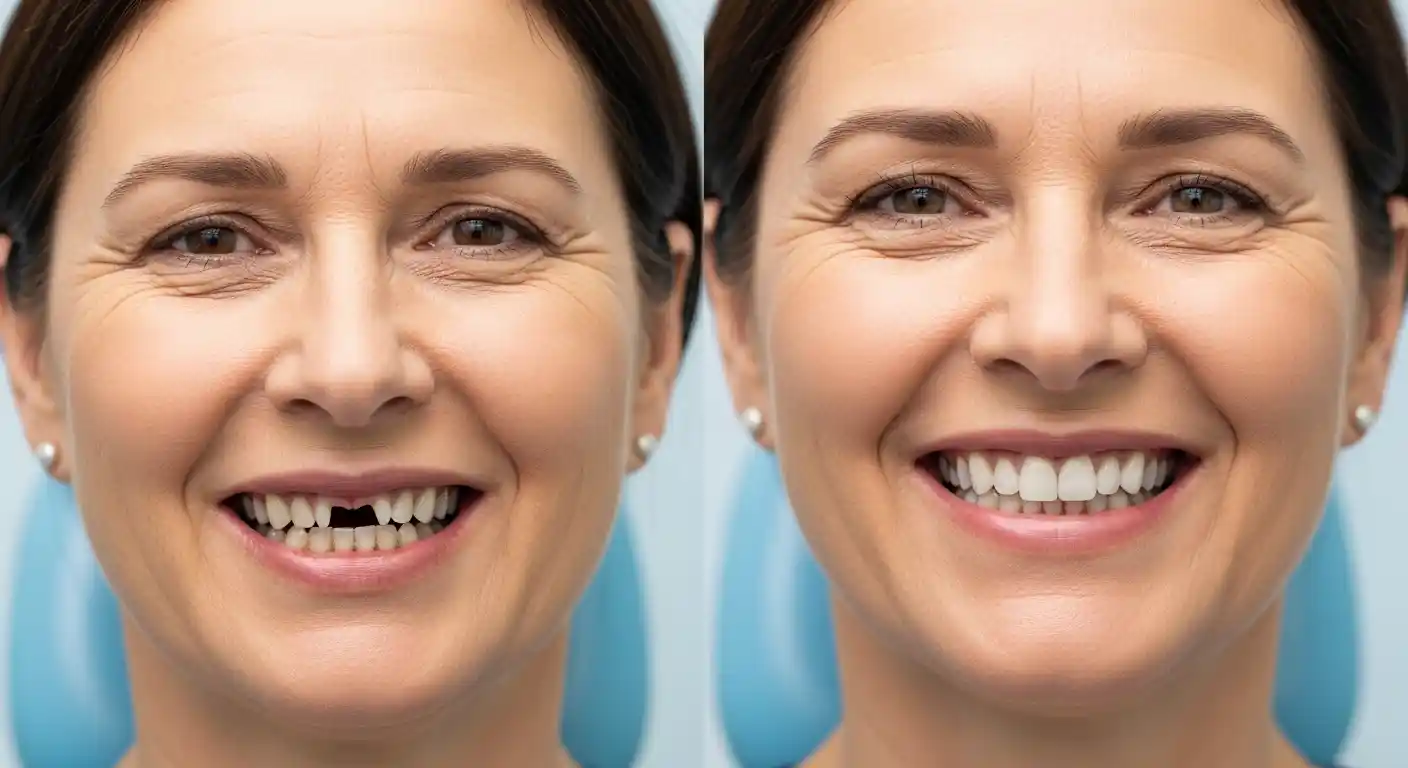
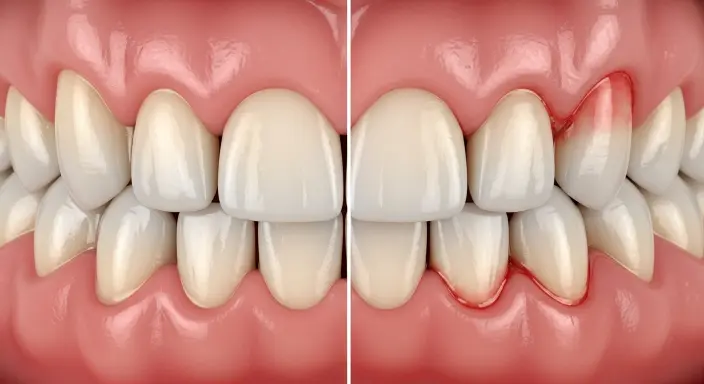
Yes, a decaying tooth can absolutely cause stomach issues—and it’s more common than you might think. When a tooth becomes infected or severely decayed, harmful bacteria can directly enter your digestive system every time you swallow, potentially triggering nausea, stomach pain, cramping, and even diarrhea a problem that residents of San Tan Valley, AZ, may particularly experience.
You swallow approximately 600 times per day, carrying bacteria from your mouth straight to your stomach. An infected tooth releases pathogenic bacteria that can overwhelm your digestive defenses and cause inflammation throughout your body. If you’ve been experiencing unexplained digestive problems alongside dental pain, your teeth might be the culprit.
Understanding Tooth Decay and Dental Infections
Before exploring how dental problems impact your stomach, it’s essential to understand what happens when a tooth decays and why infections can become serious health threats.
What Causes a Decaying or Rotting Tooth?
Tooth decay develops when bacteria in your mouth feed on sugars and starches from food, producing acids that gradually erode tooth enamel. This process begins with plaque, a sticky film of bacteria that constantly forms on teeth. Without proper brushing and flossing, plaque hardens into tartar, creating an ideal environment for decay.
Surface-level cavities may cause mild sensitivity, but deeper decay penetrates through the enamel and dentin layers, eventually reaching the tooth’s inner pulp where nerves and blood vessels reside. Poor oral hygiene, frequent snacking, sugary drinks, and inadequate fluoride exposure all accelerate this deterioration.
Symptoms of Tooth Decay and Infection
Early tooth decay often produces subtle symptoms that many people dismiss. You might experience occasional sensitivity to hot, cold, or sweet foods. As decay progresses, symptoms intensify and may include persistent toothache, sharp pain when biting, visible holes in teeth, brown or black staining, and swelling in surrounding gums.
Bad breath that doesn’t improve with brushing often signals bacterial overgrowth from decay. Many dental infections develop gradually without obvious pain, particularly when the tooth’s nerve has died. This absence of pain creates a false sense that nothing is wrong, even as infection spreads beneath the surface.
What Is a Tooth Abscess?
A tooth abscess represents the most serious complication of untreated decay. When bacteria penetrate deep into the tooth’s pulp chamber, they trigger an infection that the body tries to contain by forming a pocket of pus.
Abscesses can form at the tooth’s root tip or in the surrounding gum tissue. The real danger lies in bacterial proliferation—an untreated abscess doesn’t simply stay localized. Bacteria can enter the bloodstream or lymphatic system, potentially affecting distant organs including your digestive tract.
The Mouth–Stomach Connection Explained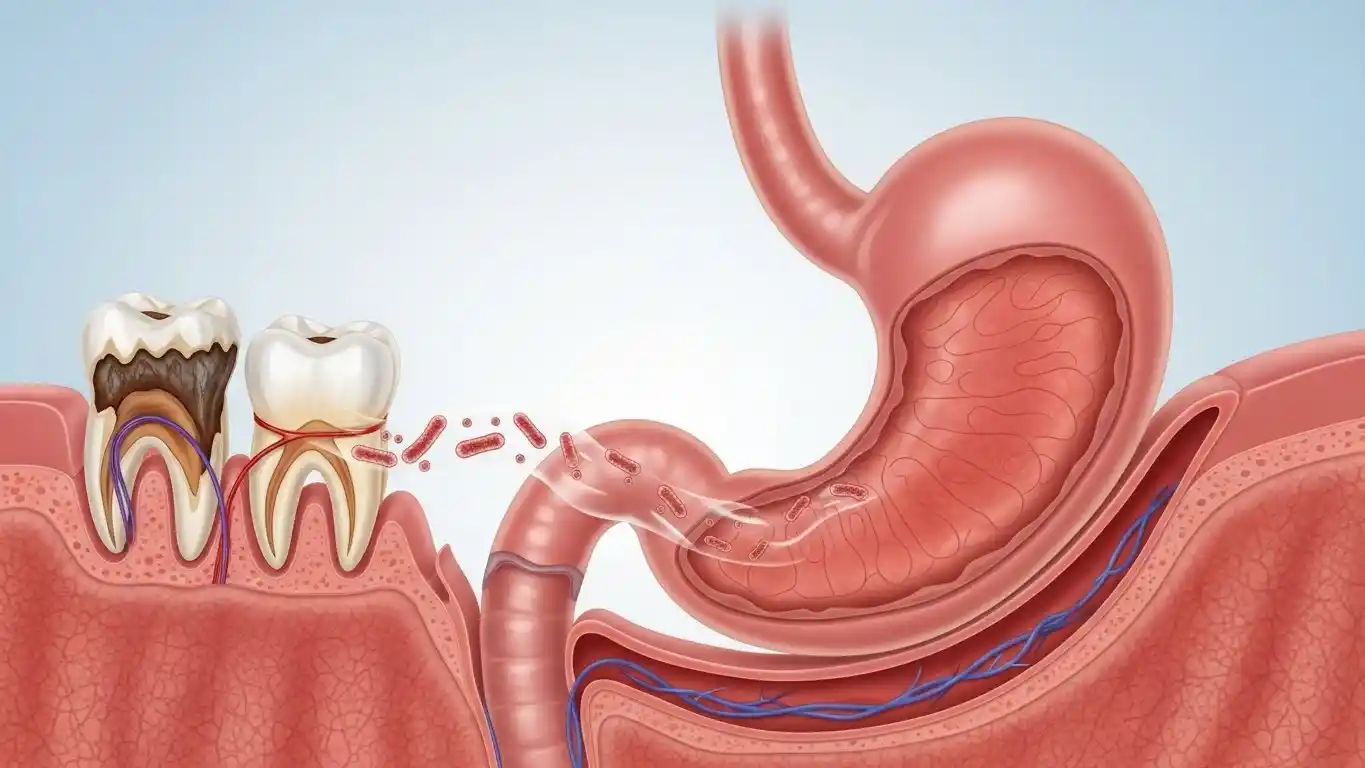
Your mouth and stomach are directly connected through your digestive tract, creating a biological highway for bacteria to travel from oral infections to your gut.
The Mouth as the First Step in Digestion
Digestion begins the moment food enters your mouth. Your teeth mechanically break down food while salivary glands release enzymes that start chemical breakdown of starches. When tooth decay or infection disrupts this environment, harmful bacteria flourish unchecked.
Each time you swallow—which happens approximately 600 times daily—you transport whatever exists in your mouth down to your stomach. An infected or decaying tooth introduces pathogenic bacteria in much higher concentrations, overwhelming your digestive system’s natural defenses.
How Oral Bacteria Reach the Stomach
The most direct route for oral bacteria to reach your stomach is through swallowing. When a tooth harbors infection, each swallow delivers harmful bacteria and their toxic byproducts directly into your digestive tract.
Additionally, dental infections that cause bleeding gums or abscesses create openings where bacteria can enter your bloodstream. Research shows that specific oral pathogens have been found in stomach tissue and intestinal biopsies of patients with digestive disorders.
Inflammation and Digestive Disruption
Your immune system responds to bacterial infection by triggering inflammation. While this response protects you, chronic inflammation from an ongoing dental infection creates collateral damage. Inflammatory chemicals circulating in your bloodstream can irritate the stomach lining, increasing acid production and sensitivity.
This systemic inflammation also disrupts the delicate balance of your gut microbiome. When harmful oral bacteria colonize your digestive tract, they compete with beneficial species, potentially leading to dysbiosis and various digestive symptoms.
Can a Decaying Tooth Really Cause Stomach Issues?
The scientific evidence supporting the connection between dental infections and digestive problems continues to grow. Studies show that individuals with poor oral health experience higher rates of gastrointestinal disorders compared to those with healthy teeth and gums.
Chronic dental infections create a persistent source of bacterial exposure that your digestive system must constantly combat. The immune response to dental infection doesn’t remain localized—inflammatory cytokines produced in response to oral bacteria circulate throughout your body, potentially triggering symptoms far from their source.
Perhaps the most compelling evidence comes from patients who experience resolution of unexplained stomach issues after treating dental infections. Dentists and gastroenterologists increasingly recognize cases where persistent digestive complaints dramatically improve following tooth extraction, root canal therapy, or antibiotic treatment for dental abscesses.
Common Stomach Issues Linked to a Decaying Tooth
Dental infections can manifest as various digestive symptoms, many of which people never suspect originate from their mouth. Recognizing these specific stomach problems helps you identify whether your digestive complaints might have a dental source.
Nausea and Vomiting
Nausea represents one of the most common stomach complaints associated with dental infections. When you continuously swallow bacteria and their toxic waste products from an infected tooth, your stomach may react defensively, triggering nausea as a protective response.
Additionally, your immune system’s response to infection can stimulate nausea centers in your brain. Inflammatory chemicals and bacterial toxins in your bloodstream can directly affect areas of the brain that control vomiting reflexes.
Stomach Pain and Cramping
Abdominal pain linked to dental infection typically presents as generalized discomfort or cramping. The inflammation triggered by chronic bacterial exposure irritates the stomach lining, potentially causing gastritis-like symptoms.
Chronic pain from dental infection also activates your body’s stress response, increasing production of stress hormones that affect digestion. These hormones can alter stomach acid secretion, slow gastric emptying, and create tension in abdominal muscles.
Diarrhea or Digestive Upset
When harmful bacteria from your mouth colonize your intestines, they disrupt the delicate microbial balance necessary for healthy digestion. This dysbiosis can impair nutrient absorption, increase intestinal permeability, and trigger loose stools or diarrhea.
Interestingly, antibiotic treatment for dental infections can also cause temporary diarrhea by killing both harmful and beneficial gut bacteria. However, untreated dental infections create ongoing bacterial challenges that perpetuate digestive upset.
Loss of Appetite and Dehydration
Dental pain often makes eating uncomfortable or impossible, naturally reducing appetite. The act of chewing with a decayed or infected tooth can cause sharp pain, leading many people to avoid meals or choose only soft foods.
Systemic infection from a dental abscess frequently causes fatigue, malaise, and decreased appetite as your body diverts energy toward fighting infection. When combined with nausea or vomiting, these symptoms can lead to dehydration, which further compromises digestive function.
Signs a Dental Infection May Be Affecting Your Whole Body
Certain warning signs indicate that a tooth infection has progressed beyond a localized dental problem and begun affecting your overall health. Recognizing these systemic symptoms is crucial because they signal that immediate professional intervention is necessary to prevent serious complications.
Fever, Fatigue, and Feeling Unwell
Low-grade fever often accompanies dental infections as your immune system responds to bacterial invasion. This malaise reflects your body’s systemic response to infection, with inflammatory chemicals circulating through your bloodstream affecting energy levels and comfort.
Persistent fatigue without other obvious causes should prompt consideration of hidden infections, including dental abscesses. Your immune system consumes considerable energy fighting chronic infection, leaving you feeling depleted.
Facial or Jaw Swelling
Visible swelling in your face, jaw, or neck signals that infection has spread beyond the tooth itself into surrounding tissues. This represents a dental emergency requiring immediate attention. The swelling indicates that your body cannot contain the infection.
Any facial swelling associated with tooth pain warrants urgent dental evaluation, as the infection’s proximity to your brain, eyes, and airway creates potential for serious complications.
Persistent Stomach Pain Without Digestive Cause
If you’ve undergone extensive testing for digestive problems without finding a clear gastrointestinal cause, dental infection deserves consideration. Many people see gastroenterologists for unexplained stomach pain and receive diagnoses like “functional dyspepsia” without improvement.
The mouth remains overlooked in digestive evaluations despite clear anatomical connections. If you have known dental problems or haven’t seen a dentist recently, a comprehensive dental examination should be part of investigating mysterious stomach issues.
Can Gum Disease or Bad Teeth Affect Gut Health?
While this article focuses primarily on tooth decay, gum disease presents similar risks for digestive health. Periodontal disease creates chronic inflammation and bacterial overgrowth in gum pockets around teeth. These bacteria enter your bloodstream through bleeding gums and travel to your digestive tract.
Research has identified specific periodontal bacteria in intestinal biopsies of patients with inflammatory bowel disease. Multiple missing teeth or widespread decay creates numerous sites where bacteria accumulate, constantly seeding your digestive tract with pathogenic organisms. Over time, this bacterial pressure can shift your gut microbiome toward an unhealthy composition associated with various digestive disorders.
When to See a Dentist or Doctor
Knowing when dental problems require professional attention can prevent both oral and systemic complications from worsening. Don’t wait for dental pain to become unbearable or stomach issues to severely impact your quality of life before seeking help—early intervention produces the best outcomes.
Warning Signs You Should Not Ignore
Seek dental care promptly if you experience severe or persistent tooth pain that doesn’t respond to over-the-counter pain relievers. Visible holes, chips, or dark spots on teeth indicate active decay requiring treatment.
Any facial or jaw swelling constitutes a dental emergency, as does fever accompanied by tooth pain. If you develop difficulty swallowing, breathing problems, or swelling that extends down your neck, seek emergency medical attention immediately.
Stomach symptoms combined with dental problems should prompt evaluation, especially if nausea, stomach pain, or digestive upset worsens after eating or seems connected to dental pain episodes.
Why Delaying Dental Care Can Worsen Stomach Issues
Dental infections don’t improve on their own. Without treatment, decay progresses deeper, bacterial populations grow larger, and the infection’s impact on your overall health intensifies.
The longer infection persists, the more firmly harmful bacteria establish themselves in your gut, making restoration of normal digestive function more difficult even after dental treatment. A cavity caught early might require only a simple filling, while delayed treatment could necessitate root canal therapy or extraction.
How to Prevent Stomach Issues Caused by Tooth Decay
Prevention strategies focus on maintaining excellent oral health and addressing dental problems promptly when they arise. Taking proactive steps to protect your teeth ultimately protects your digestive system and overall health from the cascade of complications that untreated dental disease can trigger.
Treat Tooth Decay Early
Schedule regular dental checkups so cavities can be detected and filled while still small. If your dentist recommends treatment, follow through promptly rather than waiting for pain to develop.
When decay has reached the tooth’s pulp, root canal therapy can often save the tooth while eliminating infection. In cases where teeth cannot be saved, extraction removes the infection source, allowing your body to heal.
Maintain Strong Oral Hygiene
Brush your teeth at least twice daily using fluoride toothpaste, spending two minutes each session. Floss daily to remove plaque and food particles from between teeth where brushes cannot reach.
Consider using an antimicrobial mouthwash to reduce bacterial populations. Limit sugary snacks and beverages, as frequent sugar exposure feeds decay-causing bacteria.
Regular Dental Checkups
Professional cleanings remove tartar that brushing cannot eliminate, preventing the bacterial buildup that leads to decay and gum disease. Most people benefit from dental visits every six months.
Dental examinations catch problems early, often before symptoms develop. X-rays reveal decay between teeth or beneath existing fillings where visual inspection cannot detect it.
Don’t Let a Decaying Tooth Compromise Your Health
If you’re experiencing dental pain or unexplained stomach issues, don’t wait for the problem to worsen. At Santan Dentist, our experienced team can diagnose and treat dental infections before they affect your entire body. Get a comprehensive dental examination and take the first step toward better oral and digestive health with our convenient online scheduling. Book Your Online Appointment Now and protect your overall wellness. Or visit us at 40815 N Ironwood Rd #102, San Tan Valley, AZ, to protect your overall wellness.
Conclusion
The connection between oral health and digestive wellness represents an important aspect of whole-body health that deserves greater recognition. A decaying tooth is not merely a dental problem confined to your mouth—it can create systemic effects that manifest as stomach pain, nausea, and digestive disturbances.
If you’re experiencing unexplained stomach issues, especially in combination with dental symptoms, consider that your mouth might be the source. Seeking prompt dental evaluation and treatment at Santan Dentist in San Tan Valley, AZ protects not only your smile but your overall health. Remember that prevention remains the best strategy—maintaining excellent oral hygiene and addressing dental problems early prevents complications that can affect your digestive system and beyond.
Frequently Asked Questions
Can a tooth infection cause stomach pain?
Yes, a tooth infection can cause stomach pain through multiple mechanisms. Bacteria from the infected tooth enter your stomach when you swallow, potentially irritating the stomach lining. The systemic inflammation triggered by dental infection can also make your stomach more sensitive.
Can a bad tooth make you feel nauseous?
A bad tooth frequently causes nausea, especially when infection is present. Your body may trigger nausea as a protective response to the bacteria and toxins you’re swallowing from the infected area.
Can tooth decay cause diarrhea?
Tooth decay can contribute to diarrhea when harmful oral bacteria colonize your intestines and disrupt your gut microbiome balance. This bacterial imbalance can impair normal digestion and increase intestinal motility.
Will treating a decayed tooth fix stomach issues?
Many people experience significant improvement or complete resolution of stomach issues after treating dental infections. However, if the infection has disrupted your gut microbiome, digestive symptoms may take several weeks to fully resolve.
Can a tooth infection cause acid reflux or heartburn?
Yes, a tooth infection can contribute to acid reflux or heartburn. Swallowed bacteria and inflammation may irritate the stomach lining and increase acid production, leading to reflux symptoms.